The study, published yesterday in the journal PLoS Biology, provides the first plausible explanation for how one of the world’s deadliest diseases came to infect humans.
The findings could help researchers find new ways to fight malaria and also improve their understanding more generally of how pathogens switch from one species to another.
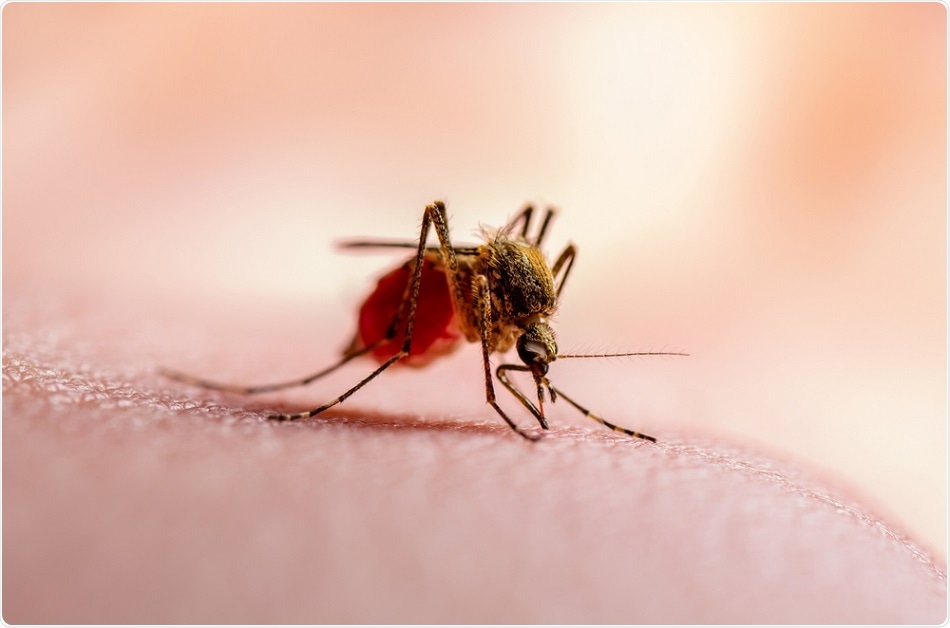
Almost half of the world’s population is at risk of malaria infection
Malaria is caused by a parasite that gets into the bloodstream when an infected mosquito bites a human or animal host.Almost half of the world’s population is at risk of infection, with the majority of cases occurring in young children in sub-Saharan Africa. This major global health problem is responsible for around 435,000 deaths every year, 61% of which are among children under five years old.
There are many different strains of the parasite, but the most deadly species is Plasmodium falciparum. This species is particularly prevalent in Africa, where it accounted for almost all (99.7%) of malaria cases in 2017.
The researchers say P.falciparum jumped from apes at approximately the same time humans first migrated out of Africa, around 40,000 to 60,000 years ago.
"This was a very rare event that led to so much death and disease in humans,” said lead author Gavin Wright from the Wellcome Sanger Institute.
The Laverania subgenus
P. falciparum is one of seven species of malaria parasites within the subgenus Laverania. These species originated in African great apes, but are now confined to their own specific hosts, with three restricted to chimpanzees and three to gorillas. The seventh strain, P. falciparum, now only infects humans after having jumped from apes about 50,000 years agoGenome sequencing of the seven Laverania strains revealed a DNA sequence that had transferred from the gorilla-infecting parasite Plasmodium adleri to an ancestor P.falciparum. This section of DNA included a gene called rh5 that encodes a protein (RH5) that binds to a receptor on human red blood cells. The protein receptor is called basigin.
This binding represents a promising basis for designing vaccines - if the interaction could be prevented, the parasite would no longer be able to infect human cells.
Reconstructing the vital rh5 sequence
To investigate the origin of P.falciparum further, researchers at the University of Montpellier reconstructed the vital rh5 sequence that transferred to the Plasmodium adleri ancestor. Wright and colleagues at Wellcome then created synthetic copies of the ancestral gene and studied the molecular interactions of the RH5 protein.They had expected that RH5 would only bind to basigin on gorilla cells, but instead, they found it binded to the receptor in both gorillas and humans. This immediately explained how the parasite switched host on a molecular level.
We were quite surprised by the findings. It was very satisfying because it makes sense with lots of other research that has been done by colleagues. It provides this molecular explanation now as to how this jump could have occurred."
Gavin Wright
A mutation was identified that explained how the parasite became restricted to humans
Next, the team identified six differences between the ancestral rh5 gene and the one currently found in P.falciparum. They found that one of the mutations resulted in a complete loss of the protein’s ability to bind basigin in gorillas, which then explained how the parasite became confined to humans.“It’s fascinating to be able to ‘resurrect’ ancestral genes such as the one which allowed Plasmodium falciparum to jump from gorillas to humans. We’ve discovered not only how a species host switch has occurred, but the individual mutation which has then restricted P. falciparum to a single host species,” said co-lead author Franck Prugnolle from the University of Montpellier.
This type of introgression event that seems to have resulted in P. falciparum switching host is extremely rare. Among the seven Laverania strains, genomic analysis has revealed just a few cases of a gene transferring from one parasite to another over a timeframe of about one million years.
In the history of mankind, Plasmodium falciparum malaria has arguably been responsible for more human deaths than any other disease. So it is both important and fascinating to understand the molecular pathways that enabled this deadly parasite to infect humans."
Gavin Wright
"Rh5 currently is an important blood stage vaccine candidate for malaria and so if we can get any more information on this gene, that could really help us in trying to combat this disease," he concludes.
Journal reference:
Resurrection of the ancestral RH5 invasion ligand provides a molecular explanation for the origin of P. falciparum malaria in humans. Francis Galaway et al. Published October 15, 2019. PLOS Biology. https://doi.org/10.1371/journal.pbio.3000490.






No comments
Post a Comment